Across continents and time zones, the modern traveller has perfected the art of external movement. We cross oceans with composure, dine adventurously, negotiate climates, cultures and cuisines with cultivated ease. Yet while our passports accumulate stamps, the body keeps its own record; and it is far less forgiving. Among the most discreet yet disruptive ailments that can shadow a life of motion is the peptic ulcer
By Olabisi Oyelowo
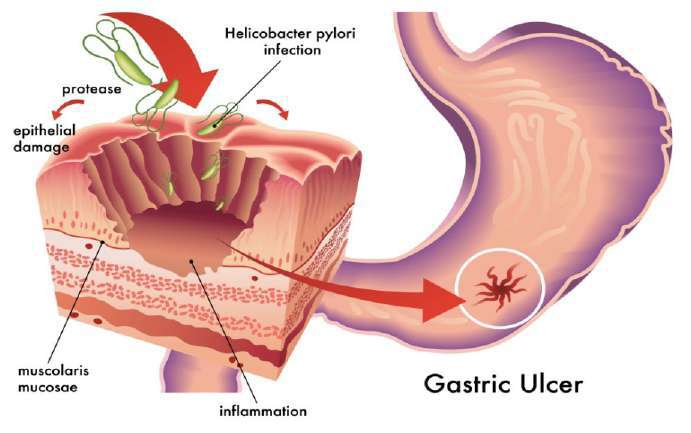
An ulcer, whether gastric or duodenal, is a lesion in the lining of the stomach or upper small intestine, often linked to Helicobacter pylori infection, prolonged use of certain pain medications, excess acid production, or chronic physiological stress. For the sophisticated traveller whose calendar is full and whose ambitions are global, the condition can be both inconvenient and humbling. Left unmanaged, it may intrude upon pleasure, compromise performance, and diminish vitality.
Yet an ulcer is not a verdict. With disciplined care, intelligent adjustment, and a certain elegance of self-regard, it can be managed, and in many cases, conquered. What follows are seven refined principles for restoring digestive equilibrium and reclaiming health without sacrificing the richness of a well-travelled life.


1. Seek Precision Before Prescription
The cultivated mind does not confuse symptoms with conclusions. Abdominal discomfort, burning pain, bloating or nausea may suggest an ulcer; but they may equally signal reflux disease, gallbladder disorders, gastritis, or functional dyspepsia. The first act of mastery, therefore, is diagnostic clarity.

Consultation with a qualified physician is indispensable. Testing may include non-invasive screening for H. pylori, blood work, or, where necessary, endoscopy. If infection is confirmed, a structured course of antibiotics combined with acid-suppressing therapy can often achieve eradication. If medication overuse is implicated, particularly non-steroidal anti-inflammatory drugs, alternatives must be discussed. If acid hypersecretion is the driver, proton pump inhibitors or H2 blockers provide a highly effective therapeutic bridge to healing.
For the frequent traveller, timing matters. Whenever possible, initiate evaluation and treatment before embarking on extended journeys. Carry medical documentation digitally. Travel with adequate medication supplies in original packaging. Identify reputable medical facilities at your destination; not out of anxiety, but out of prudence.
Self-medication with antacids alone may provide temporary relief, but it risks masking a deeper pathology. True sophistication in health begins with respect for evidence. An ulcer managed on assumption is an ulcer invited to persist. Precision is the first step toward conquest.
2. Restore Rhythm to Eating
The stomach is not designed for chaos. Irregular meals, long fasts punctuated by indulgent feasts, destabilize acid secretion and strain already vulnerable tissue. In the cultivated life, rhythm is not restriction; it is refinement.
Adopt predictable meal intervals. Smaller, balanced portions taken consistently throughout the day allow the stomach to function without dramatic surges of acid. Lean proteins, whole grains, gently cooked vegetables, and non-acidic fruits provide nourishment without unnecessary irritation. While tolerance varies, heavily fried, excessively spicy, or highly acidic dishes often provoke symptoms in active ulcer disease.
For the international epicurean, moderation is the watchword. Share courses. Pair richer dishes with soothing staples such as rice or steamed greens. Avoid late-night dining after prolonged fasting. Eat slowly; not as performance, but as presence. Chewing thoroughly reduces gastric burden and signals satiety before excess accumulates.
Hydration should be steady rather than sporadic. Excess caffeine, particularly on an empty stomach, may aggravate symptoms. Replace one coffee with herbal tea; substitute carbonated beverages with still water.
The aim is not culinary austerity but digestive civility. When meals become deliberate rather than impulsive, the stomach is granted an environment in which healing becomes possible. Rhythm restores order, and order restores strength.
3. Govern Stress with Intention
Once blamed entirely for ulcers, stress is now understood not as sole cause but as potent accomplice. Chronic stress elevates acid production, impairs mucosal defense, alters gut motility, and compromises immune resilience. In other words, it creates an internal climate in which healing struggles to take root.
The internationally engaged individual is rarely untouched by pressure. Negotiations, deadlines, flights across time zones, public expectations: these are the currencies of influence. Yet the nervous system responds to psychological strain as though it were physical threat.
Mastery begins with awareness. Identify patterns: does pain intensify during travel? Before presentations? After prolonged sleep deprivation? Such recognition transforms suffering into data.
Incorporate daily practices that regulate the autonomic nervous system. Controlled breathing exercises, meditation, restorative yoga, contemplative walking in unfamiliar cities; these are not indulgences but biological interventions. Guard sleep with discipline. Eight hours of restorative rest recalibrates hormonal balance and supports tissue repair.
When travelling, build margins into schedules. Resist compressing itineraries to the point of exhaustion. The world will still be there tomorrow; your mucosa may not.
To govern stress is not to abandon ambition. It is to exercise stewardship over it. An ulcer often signals not weakness, but imbalance. Restore equilibrium, and healing follows.



4. Reconsider Alcohol and Eliminate Tobacco
Travel often celebrates indulgence: the regional wine, the late-night cocktail overlooking an illuminated skyline. Yet alcohol is a direct gastric irritant. It inflames the lining of the stomach, increases acid secretion, and can delay ulcer healing. Tobacco compounds the injury by reducing blood flow to gastric tissue and increasing recurrence rates.
For those managing an active ulcer, temporary abstinence from alcohol is wise. If and when reintroduced, it should be done cautiously, with food, and in strict moderation. Quality must replace quantity. One glass savored slowly is physiologically less disruptive than several consumed quickly on an empty stomach.
Smoking cessation, by contrast, should be absolute. Beyond its systemic harms, tobacco markedly impairs ulcer healing and increases complications. There is no elegant compromise here.
Declining excess is not a diminishment of pleasure. It is an elevation of discernment. The refined traveller understands that vitality enhances every experience; from tasting a new cuisine to delivering a keynote address. To protect the stomach is to protect the self that experiences the world.
Restraint, in this context, is not austerity. It is strategic longevity.

5. Practice Medication Fidelity
Modern ulcer therapy is remarkably effective; provided it is followed precisely. Acid-suppressing medications must often be taken before meals to maximize efficacy. Antibiotic regimens for H. pylori must be completed in full, even if symptoms resolve early. Partial adherence invites recurrence and resistance.
Time zone changes can complicate dosing schedules. Establish a clear plan before departure. Use digital reminders calibrated to destination time. Carry extra medication in case of delays. Store drugs according to recommended temperature guidelines.
Avoid casual use of non-steroidal anti-inflammatory drugs for minor aches during travel. For those with chronic pain conditions, discuss protective strategies with a physician — which may include co-prescribed acid suppression.
Medication discipline lacks romance. It requires quiet consistency rather than dramatic intervention. Yet healing is cumulative. Each correctly timed dose is a small vote cast in favor of recovery.
In the theatre of global mobility, where spontaneity is often celebrated, structured adherence may feel counterintuitive. But the stomach thrives on reliability. Fidelity to treatment is fidelity to one’s future comfort.

6. Cultivate the Internal Ecosystem
The gastrointestinal tract is not a sterile tube but a living ecosystem inhabited by trillions of microorganisms. Antibiotic therapy, though often necessary, disrupts this internal community. Restoring microbial balance supports mucosal resilience and long-term digestive health.
Incorporate probiotic-rich foods such as yoghurt with live cultures where tolerated. A diet rich in fiber from vegetables, legumes, and whole grains nourishes beneficial bacteria and enhances mucosal integrity. During and after antibiotic treatment, consult a healthcare provider about targeted probiotic supplementation.
Travel introduces additional variables. Food hygiene becomes paramount. Choose reputable establishments. Be attentive to water safety in unfamiliar regions. Hand hygiene, an unglamorous but essential discipline, reduces exposure to pathogens that may compound gastric irritation.
This is not mere nutritional fashion. It is ecological stewardship. When the internal environment is diverse and balanced, it resists invasion and supports repair.
To cultivate the microbiome is to recognize that health is symphonic rather than solitary. Harmony within permits confidence without.
7. Adopt a Philosophy of Sustained Care
Conquering an ulcer is not a singular event but an orientation. Even after symptoms subside, vigilance remains prudent. Follow-up testing may be necessary to confirm eradication of infection. Recurrent pain should prompt evaluation, not dismissal.
Sustained care involves more than medication. It is a lifestyle architecture: balanced meals, moderated indulgence, managed stress, disciplined sleep, thoughtful travel planning. It is the recognition that resilience is built daily.
The ulcer, paradoxically, can serve as teacher. It insists upon rhythm in a life inclined toward acceleration. It invites discernment in a culture that prizes excess. It demands attention in a world of distraction.
For the elevated traveller, one who values not only destinations but durability, health is not peripheral. It is foundational. The ability to walk ancient streets, negotiate complex agreements, or savor distant horizons depends upon a body functioning in quiet strength. To manage an ulcer is to reclaim sovereignty over one’s internal terrain. To conquer it is to align ambition with balance. And in that alignment lies the most enduring luxury of all: sustained vitality in a life lived expansively.





